Before I begin, I want you to know that my intention is not to put any kind of blame on you or the midwives involved on the day my beautiful girl was born. I chose to be on the midwife program at a public hospital and my midwife wasn’t working the day my baby decided to make her way into the world and that’s just the way it is.
I am writing this because I feel it is important that you know. It’s over 2 years now since my motherhood journey began and along the way, as you know, I have experienced some significant challenges after the forceps delivery and subsequent tearing. I felt compelled to write having recently heard of another woman’s experience at the same hospital where I had my daughter.
The woman who was, like me, desperate for a ‘natural’ birth faced the same forceps or c-section decision and, having been given her options and told about the risk of prolapse and incontinence, she opted for a c-section. I found myself wondering again whether, had I been informed of the risks, I would have chosen the latter. The answer isn’t 100% yes. I mean, it wasn’t until my girl was 16 months old that I truly discovered what a prolapse is!
While we all did the best we could with what we knew at the time, there are still moments when I fleetingly wonder how different it may have been had my midwife been on duty that day, had I been better informed about the risks of forceps deliveries and had I not been in labour for 19 hours, awake for about 48 hours and completely out of it. What I do know is that I can’t keep looking back, or forward. All the matters is what I do with my knowledge now.
When I found out I was pregnant, I was training for a fitness competition, fitness was my life. I think every time we met in the subsequent months after the delivery I quizzed you about the types of exercise I could do, I was so desperate to get back to lifting weights and working out in my sweat ridden gym.
I have since learnt that many new mothers who are into fitness can really struggle with the loss of endorphins that they get from exercise, making them more prone to postnatal depression.
I was considered high risk due to the fact I’d had such a traumatic birth. I have always credited exercise as one of the best anti-depressants available. On our last meeting you said that I should ‘just live the life I want and if you prolapse, you can get surgery once you’ve finished having kids’.
I took that advice and eased myself back in to the sports I loved, but the heaviness was too much, I knew things weren’t right and I finally found answers from my amazing women’s heath physiotherapist. I have a levator avulsion that has led to pelvic organ prolapse (POP). I haven’t had a scan to determine how much muscle is left attached to the bone, but my pelvic floor activation is probably only a fraction stronger since I last saw you, despite my best efforts of serious lifestyle modifications and pelvic floor training.
Based on statistics, surgery for POP has a 1 in 3 failure rate though it could be higher considering many women don’t go back to the same Doctor that performed the repair. Due to the nature of my pelvic floor damage, surgery has an even higher risk of failure, for me personally – I don’t want to be in and out of hospital for the next 30+ years.
When I mentioned to you that I was to be fitted with a pessary to help support my organs, you expressed your concern by suggesting that they are for old women who don’t have sex. Although I shouldn’t have to tell you, pessaries are much more than that. It took a while for me to adapt to mine, at first I felt so sad about having to use it feeling utterly betrayed by my own body. I used to cry so hard when I had to take it out, a hot, sweaty and weeping mess, wondering whether I would ever manage!
Over time it has gotten much easier and enables a level of normality. I actually know women that are able to have sex with their pessaries in and their hubbies are very happy indeed! I have since connected with many other women who are in their twenties, thirties and forties and who choose pessaries over surgery. Please consider this; doing everything to avoid POP is more important than thinking surgery is the solution when it happens.
I need you to know, from a mother who took a lot of time to find peace with her new body and it’s limitations that POP can have serious power over everyday life. Many women, like me, struggle with quality of life. Simple tasks that we once took for granted, like being able to lift up your toddler, run, jump or perform basic functional movements like squatting and bending, can become a constant source of worry.
Sadly it seems that a large percentage of women assume their symptoms are normal after having a child or feel ashamed and embarrassed by their condition and choose to suffer in silence, so the true mental impact of this POP is barely discussed. From first-hand experience and from talking to women who are in similar positions, depression and anxiety disorders are common, affecting not just the women suffering but their loved ones too.
That December day in 2013, my path completely shifted. I am determined to raise awareness for this unbelievably common condition, so common that studies suggest 50% of mothers will have some degree of prolapse in their lifetimes and yet most people outside of the medical profession have never even heard of, simply by starting the conversation and I can wholeheartedly thank you for giving me that voice.
Can you relate to this? Please share your experiences.
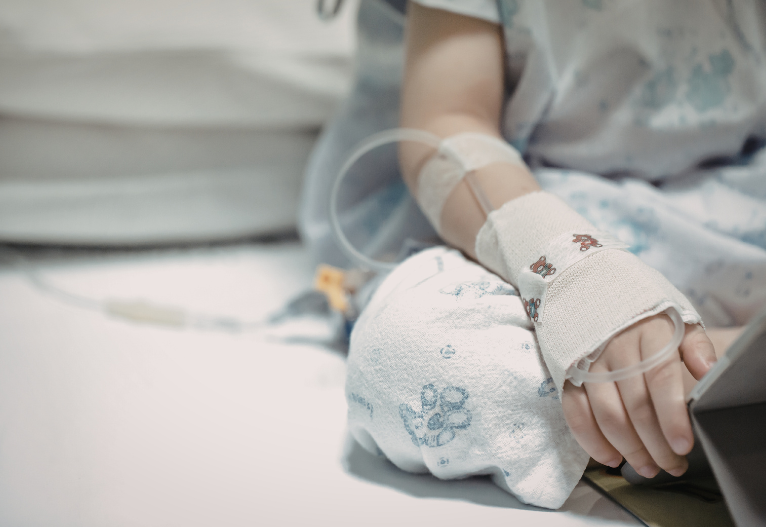
Image source: Supplied




















12:52 pm
2:58 pm
2:25 pm
9:55 pm
7:16 pm
8:43 am
1:41 pm
3:32 am
4:28 pm
8:29 pm
9:32 pm
9:42 am
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:16 pm
Reply9:29 pm
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:19 pm
-

-
-
june11 replied
- 08 Jul 2016 , 8:36 pm
Reply4:34 pm
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:20 pm
Reply2:21 pm
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:21 pm
Reply10:57 pm
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:25 pm
Reply8:30 pm
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:27 pm
Reply8:21 pm
-

-
-
Amy Dawes replied
- 07 Jul 2016 , 8:32 pm
Reply4:02 pm
-

-
-
Amy Dawes replied
- 24 Jun 2016 , 5:02 pm
Reply3:14 am
-

-
-
Amy Dawes replied
- 24 Jun 2016 , 4:59 pm
Reply- 1
- 2
- 3
- »
Post a commentTo post a review/comment please join us or login so we can allocate your points.