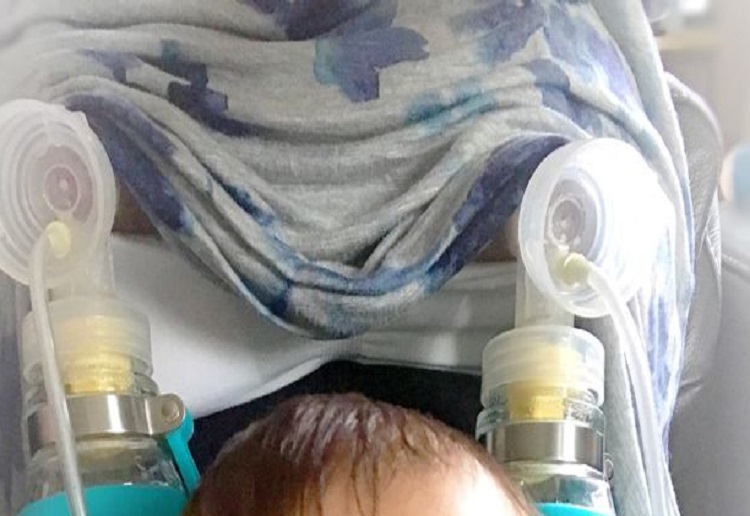
Elisabeth Anderson-Sierra, 29, spends an incredible 10 hours a day pumping around 1.75 gallons (8ltrs) of milk to help thousands of babies.
Elizabeth has been diagnosed with hyperlactation syndrome, which means she produces masses more milk than what is considered a ‘normal’ amount.
She still manages to feed her own six-month-old daughter Sophia, before generously giving the rest to those more needy than herself.
Donating the precious liquid gold to mums who struggle to breast feed, premature babies and gay dads, Elizabeth says she has fed thousands of babies, reports The mirror.
Her milk is packaged, labelled and stored in four huge freezers in the house where she lives with her two girls and her husband, David Sierra, 52.
She says producing the “liquid gold” is her “labor of love”.
Elizabeth, also mum to two-year-old Isabella, said: “I realised I was an overproducer when I was pregnant with my first child, but when I had my second baby my supply ramped up.
“Now Sophia is six months old I pump five times a day – as soon as I wake up, after breakfast, after lunch, after dinner and again at midnight.
“I produce 70 to 80oz of milk during my first pump alone.
“In total I will spend around five hours a day just pumping and then with storing, labelling, sterilizing etcetera, I easily spent eight to ten hours.
“Pumping is not fun – it is uncomfortable and it hurts – but it is my labor of love.
“I’ve not had a day off in two-and-a-half years. It’s more than a full-time job.
“It is instant gratification when I donate locally because I see the babies and I see them thriving.
“It will have helped thousands of children. The milk at the milk bank goes to micro pre-emies, so 1oz can feed three or four babies.
“I don’t discriminate – I have donated to gay couples and to mothers who are on medication or had their breast removed due to breast cancer.
“It’s an amazing feeling.”
Australian guidelines
Donor milk is a human body fluid with some accompanying risks.
These include viruses (e.g. HIV, hepatitis C), bacteria and other infectious agents such as prions (i.e. vCJD). These risks need to be kept in perspective.
While blood borne viruses are found in the breast milk of infected mothers, transmission from mother to child through breast milk is rare, and occurs at much lower rates than with blood (Gribble 2012).
Donor screening and pasteurisation reduce the risks even further. Despite a long history of milk banking internationally, reports of adverse events are extremely rare.
The risk management strategies for human milk banks cover three main stages:
• Collection of donor milk – including donor eligibility, recruitment, screening and selection (with similar criteria to blood donation); training and support for donors; and how the donor milk is expressed, stored and transported.
• Processing donor milk- including tests carried out on the milk e.g. for bacteria and nutrient composition, pasteurisation, labelling, tracking and storing (which may include freezing and thawing).
• Providing the donor milk – including recipient eligibility and prescribing of donor milk, informed consent, dispensing and feeding protocols including fortification where required, tracking and record keeping, staff training, supporting mothers to establish their own milk supply, and liability and insurance issues.
You can read more info on milk donors here
Share your comments below
Read more:
Meet the mum dedicated to provide breastmilk to total strangers
Mums turn to Facebook for breastmilk


















-

-
-
mom94125, QLD said
- 02 Sep 2017
-

-
-
june11, QLD said
- 14 Aug 2017
-

-
-
mom247592, QLD said
- 13 Aug 2017
-

-
-
hopefullyheidi, QLD said
- 31 Jul 2017
-

-
-
mom160421, QLD said
- 30 Jul 2017
-

-
-
taynik46, QLD said
- 30 Jul 2017
-

-
-
rachel1970, QLD said
- 30 Jul 2017
-

-
-
Ellen, QLD said
- 30 Jul 2017
-

-
-
BellaB, QLD said
- 29 Jul 2017
-

-
-
mom62527, QLD said
- 29 Jul 2017
-

-
-
natct, QLD said
- 29 Jul 2017
-

-
-
mum4107, QLD said
- 29 Jul 2017
-

-
-
youngoldlady, QLD said
- 28 Jul 2017
-

-
-
mom206279, QLD said
- 28 Jul 2017
-

-
-
mom90758, QLD said
- 28 Jul 2017
Post a comment8:59 pm
10:57 pm
10:24 pm
3:57 pm
3:46 pm
9:00 am
8:32 am
2:48 am
7:14 pm
12:51 pm
6:07 am
4:41 am
9:37 pm
1:24 pm
12:43 pm
To post a review/comment please join us or login so we can allocate your points.